
Recently, the research team led by Associate Professor Ke Deng from the Department of Statistics and Data Science, Tsinghua University, in collaboration with the team led by Professors Lan Zhu and Zhijing Sun from the Department of Obstetrics and Gynecology, Peking Union Medical College Hospital (PUMCH), has published a research paper addressing Pelvic Organ Prolapse (POP), a common disease plaguing women worldwide. The team developed a Multi-Dimensional Recommendation system (MUDI), which dynamically balances surgical efficacy, risks, costs, complexity and patient preference through data-driven approaches, providing transparent and personalized surgical plan recommendations for clinicians and patients. The findings were published in *npj Digital Medicine*, a top-level journal in the field of digital medicine, and the system has also obtained a national invention patent authorization.
I. From Experience-Dominated to Data-Quantified Decision-Making
The selection of surgical plans for POP is a complex process that requires a comprehensive evaluation of more than ten decision-making dimensions, including patients’ anatomical characteristics, complication risks and medical costs. Traditional methods are highly dependent on experts’ experience, and the shortage of primary medical resources makes it difficult for patients to access optimal treatment. To address the imbalance in treatment resources caused by experience-dominated decision-making, the MUDI system provides professional, transparent and convenient optimal treatment recommendations based on the rich data from PUMCH’s nearly 20-year surgical and follow-up database, combined with multi-center external validation. Its innovative breakthroughs are reflected in three aspects: (1) A multi-dimensional quantification engine that constructs surgical feature profiles covering five core dimensions: efficacy, risk, cost, complexity and patient preference; (2) Dynamic personalized recommendation that learns clinicians’ decision preferences based on clinical data, adjusts the weight of each dimension in real time, and supports a "one patient, one treatment" approach; (3) Transparent and interpretable logic where recommendation results are accompanied by quantitative evidence, intuitively demonstrating "why Plan A is chosen over Plan B" and facilitating efficient doctor-patient communication.
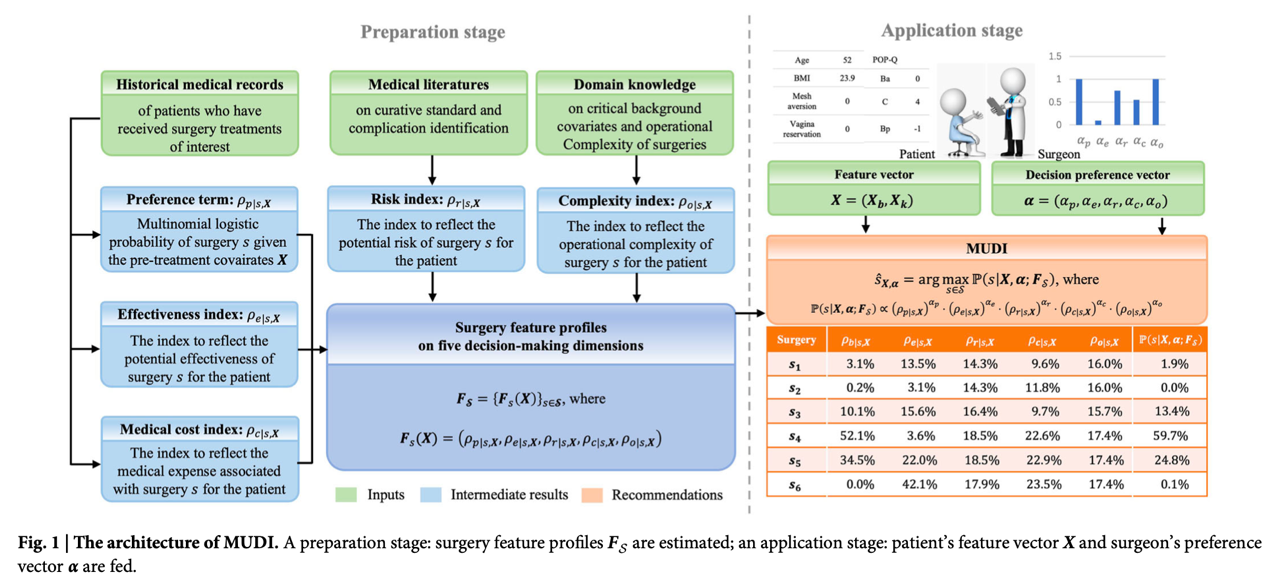
Figure 1 Core Operational Logic of the MUDI System
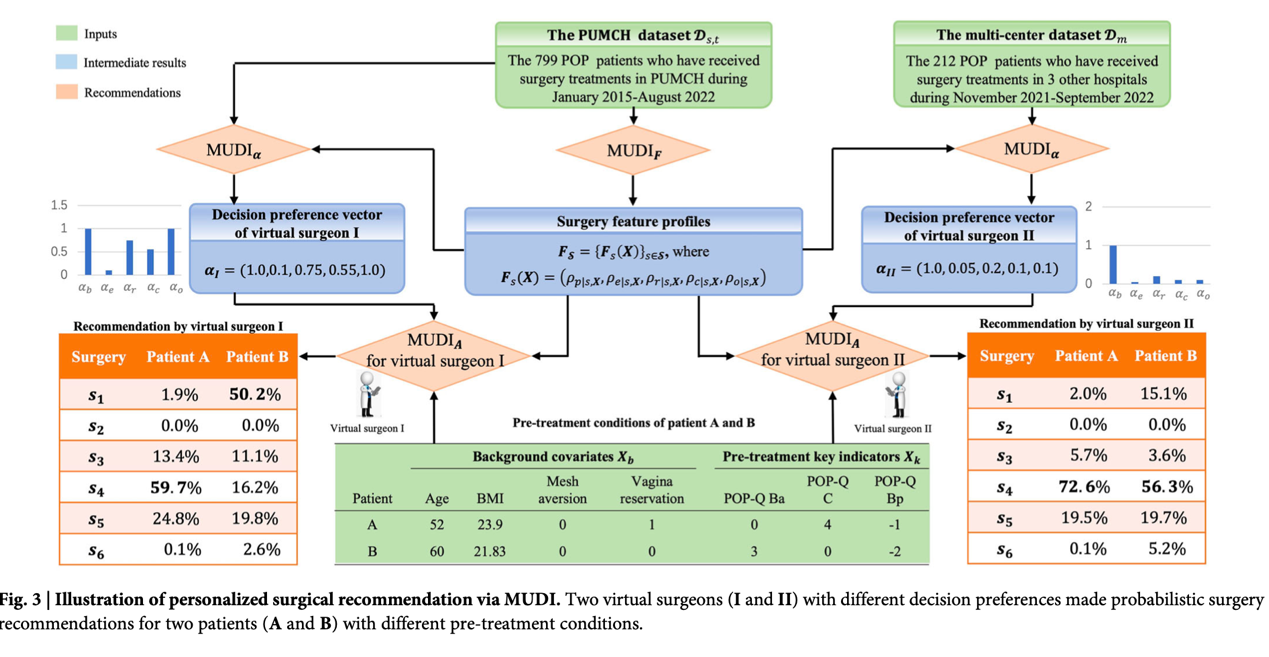
Figure 2 Personalized Treatment Recommendation by the MUDI System
II. Excellent Validation Results: Accuracy on Par with Top Experts, 27% Improvement in Primary Clinicians’ Decision-Making
The research team validated the system based on clinical data of over 1,200 POP patients from multiple domestic tertiary Grade A hospitals, with the following results: Internal Validation: The accuracy of MUDI’s Top-1 recommendation reached 60%, and the accuracy of Top-3 recommendations hit an impressive 92%; Cross-Hospital External Validation: The accuracy of Top-1 recommendation remained at 62%, on par with that of domestic top pelvic floor disease experts, and the Top-3 recommendation accuracy also reached 92%. This accuracy is significantly superior to that of general specialists (Top-1: 40%, Top-3: 81%) and primary clinicians without specialized training (Top-1: 27%, Top-3: 61%), helping to improve the surgical decision-making accuracy of primary clinicians by 21%-27%.

Figure 3: Validation Results of the MUDI System
III. Distinct Technical Advantages: From "Black Box Prediction" to Science and Logic-Driven Decision-Making
Compared with traditional machine learning models, the MUDI system demonstrates three prominent advantages: (1) Anti-overfitting for enhanced stability: The performance fluctuation was less than 2% in cross-hospital validation, while the accuracy of traditional neural network models dropped by more than 10% in multi-center validation; (2) High interpretability for improved clinician trust: In model application tests, 49%-97% of clinicians were willing to adjust their diagnostic decisions with reference to the MUDI system; (3) Flexible expandability for strong generalization: The system framework supports the addition of new decision-making dimensions (e.g., postoperative sexual function protection, postoperative rehabilitation cycle), and can be quickly migrated to other disease fields or more complex clinical treatment decision-making scenarios.
IV. Accessible Clinical Implementation: Open Online Platform Empowers Primary Healthcare
To facilitate rapid clinical implementation, the research team has simultaneously launched the MUDI online platform. When making surgical decisions for POP, primary clinicians can directly access the webpage to use functions such as one-click plan recommendation, dynamic doctor-patient interaction and medical knowledge base linkage. Assisted by the system, primary clinicians can make better and more personalized surgical decisions, enabling more primary patients to access high-level medical services consistent with those of tertiary Grade A hospitals.
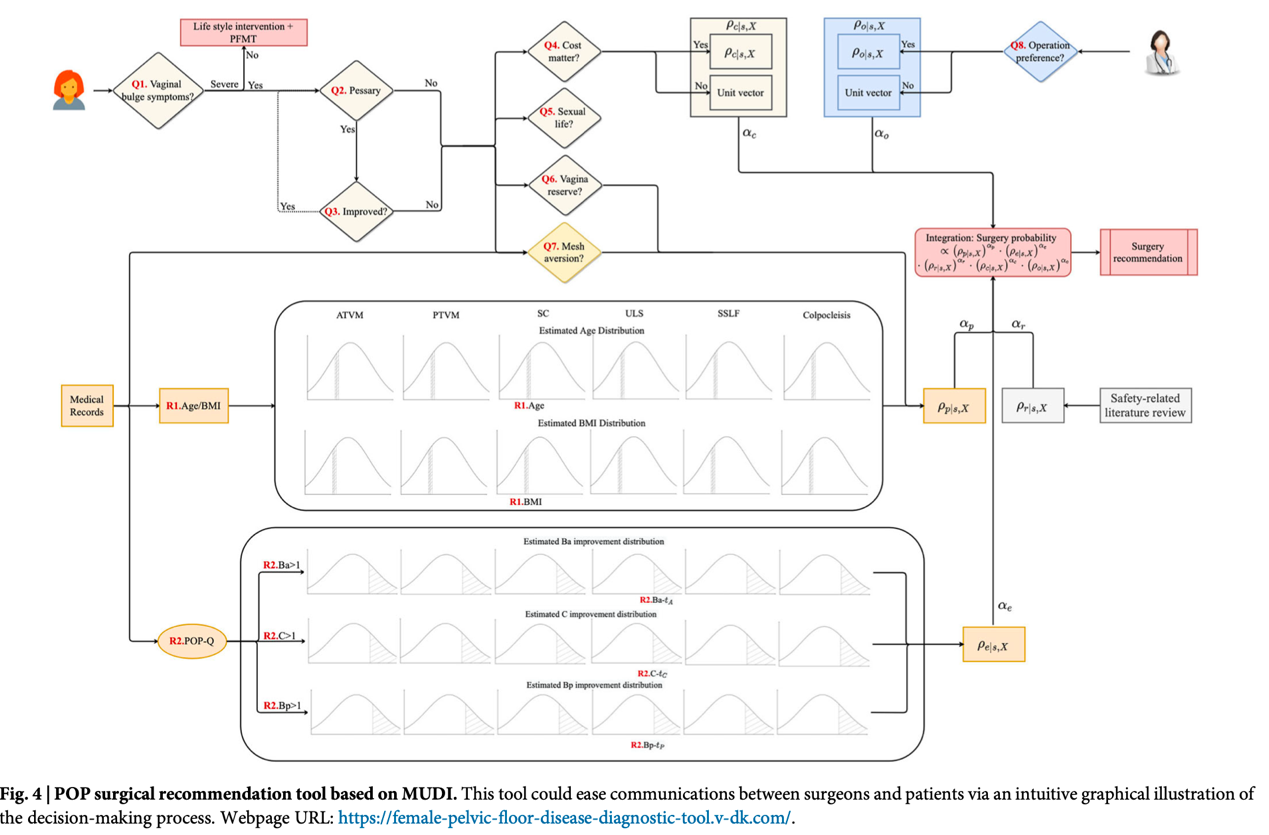
Figure 4: Open Online Platform
Link:https://www.nature.com/articles/s41746-025-01509-1

